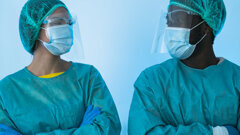
LEIPZIG, Germany: Owing to mask supplies fast becoming exhausted, many healthcare professionals around the world are increasingly unable to comply with the recommended infection control practices. The shortage has prompted extended use and reuse of face masks in healthcare settings, thus increasing the professionals’ risk of contracting SARS-CoV-2. To help ease the depleted supplies, many federal agencies have relaxed regulations on mask use and some institutions have taken the initiative to help those fighting on the front line against COVID-19 by producing 3D-printed face masks and shields.
In new guidance, the U.S. Food and Drug Administration (FDA) has relaxed regulations on medical and surgical masks and face shields and approved the use of improvised face masks in the case that no FDA-cleared masks are available. Similarly, the British government has extended the recommended wearing time and necessity of changing of face masks to better protect healthcare workers from SARS-CoV-2.
Additionally, some branches of the military have made efforts to support infection control and relieve face mask shortages. For example, the U.S. Air Force is using 3D printers to produce reusable plastic N95 face masks for medical personnel. It is also producing face shields to extend the time of use of face masks.
In response to the crisis, many universities and dental schools, such as the LSU Health New Orleans School of Dentistry in the US, too have started producing 3D-printed protective gear that is generally reusable, for donation to healthcare professionals. Taking it one step further, some dentists are developing face masks that can be constructed with items found in the dental surgery.
Commenting on the situation, Prof. Chris Whitty, chief medical officer for England, said in a press release: “It is absolutely right that front-line staff have the appropriate PPE [personal protective equipment] so they are safe and can have the confidence they need to do their jobs.”
World Health Organization’s advice on the use of face masks
In a recent publication, the World Health Organization (WHO) stated that it does not support the recommendation for healthy people to wear masks in the community setting, saying that “there is currently no evidence that wearing a mask (whether medical or other types) by healthy persons in the wider community setting, including universal community masking, can prevent them from infection with respiratory viruses, including COVID-19”.
Similarly, the Centers for Disease Control and Prevention stated on its website: “In settings where facemasks are not available, healthcare personnel might use homemade masks (e.g., bandana, scarf) for care of patients with COVID-19 as a last resort. However, homemade masks are not considered personal protective equipment (PPE), since their capability to protect healthcare personnel is unknown. Caution should be exercised when considering this option.” It added that homemade masks should be used together with a face shield that covers the entire front and the sides of the face.
“The use of medical masks in the community may create a false sense of security, with neglect of other essential measures, such as hand hygiene practices and physical distancing, and may lead to touching the face under the masks and under the eyes, result in unnecessary costs, and take masks away from those in healthcare who need them most, especially when masks are in short supply,” the WHO continued.
The WHO is currently collaborating with research and development partners to gain a better understanding of the effectiveness and efficiency of non-medical masks. Until then, decision makers have been permitted to advise the use of non-medical masks, making sure that features such as the number of layers of fabric or tissue, breathability of the material, water repellence or hydrophobic qualities, and the shape and fit of masks are being considered. Besides hand cleaning and social distancing, the WHO has recommended that all healthcare providers wear proper protective gear.
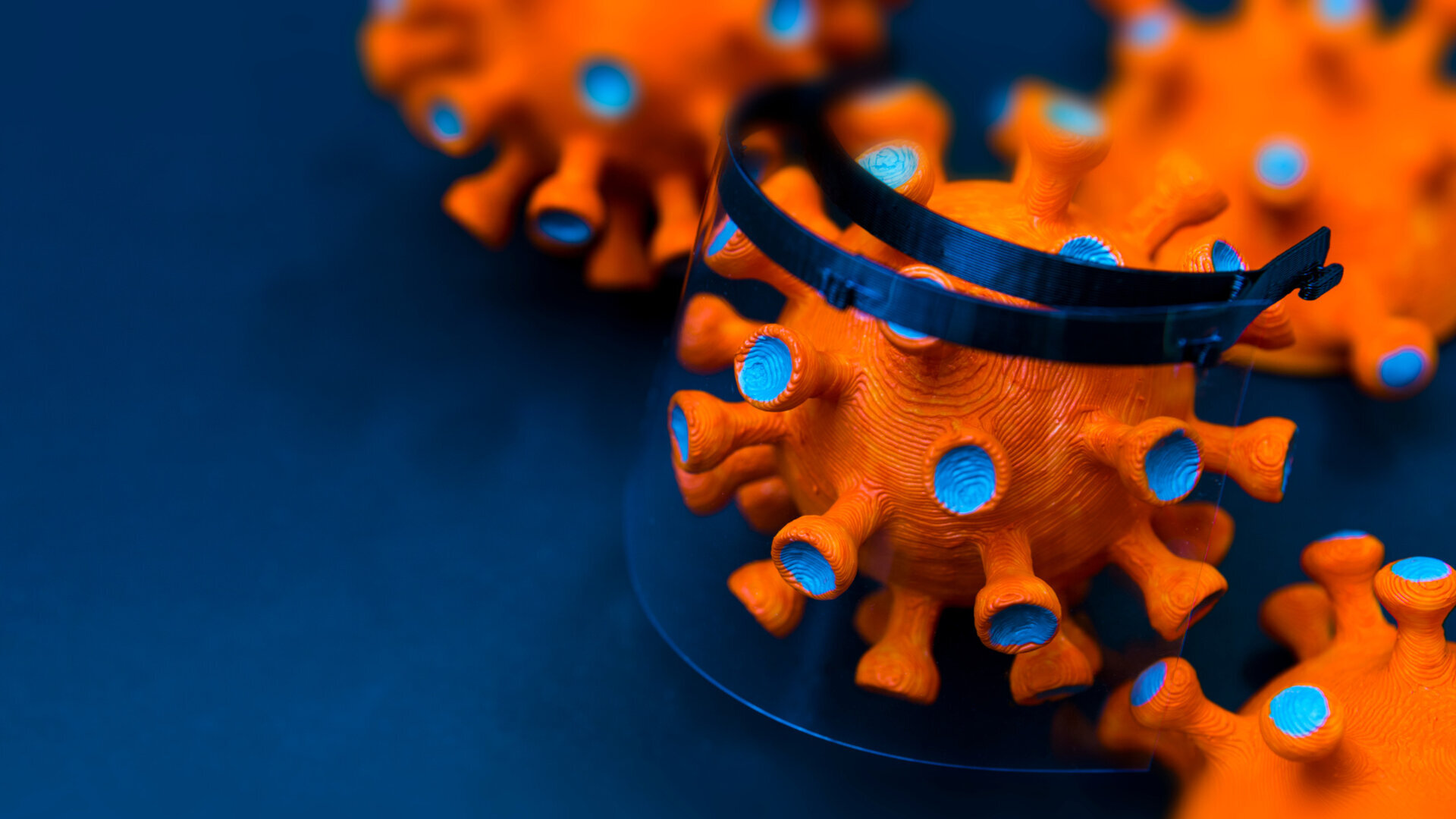
3D-printed face masks on the rise
In order to help fight the crisis and assure the safety of healthcare professionals, 3D-printed masks are now available globally. These masks are based on facial scanning, 3D imaging and 3D printing and consist of two 3D-printed reusable polyamide composite components, a face mask and a filter membrane support produced with the help of CAD. Additionally, the masks employ a disposable head fixation band and a filter membrane, both available from industrial manufacturers producing FFP2/3 protective masks, according to a research article.
In the article, the researchers note that clinical testing, including dermatological considerations, leakage and virological testing of the reusable components of the masks, has not been performed yet. This, according to them, is crucial before use, as are proper cleaning and disinfection control.
Effectiveness of surgical and cotton masks in preventing contamination
Both surgical and N95 masks have been shown to be effective in preventing influenza virus transmission. However, the effectiveness of surgical and cotton masks, which are becoming increasingly popular, in blocking SARS-CoV-2 transmission has been little studied. Aiming to fill the gap in the literature, a recent study compared the effectiveness of both types of masks in four patients with COVID-19. The patients were admitted to negative-pressure isolation rooms and instructed to cough on to a Petri dish while wearing each mask or no mask at all. After swabbing the inner and outer mask surfaces to check viral loads, the researchers found that all swabs from the outer mask surfaces were positive for SARS-CoV-2, while the majority of the swabs from the inner mask surfaces were negative. The findings suggest that neither mask type was able to effectively filter SARS-CoV-2 particles during coughs.
Assuming all dental patients are SARS-CoV-2-positive
In a recent discussion, Prof. Thomas Benton Dodson, chair of the oral and maxillofacial surgery department at University of Washington School of Dentistry in the US, said that he has advised his staff to treat every patient as if he or she has contracted SARS-CoV-2 with regard to the use of PPE. However, Dr Samir Mehta, an orthopaedic surgeon in Philadelphia in the US, said that taking such precautions is highly problematic owing to existing PPE shortages.
All the speakers agreed that there is an overwhelming amount of information coming in every day and guidelines are changing dynamically. Additionally, dentists have little time to conduct clinical trials, as they need to make immediate decisions to ensure the best possible care. As Dodson stated, dental professionals are trying to fly an aeroplane they are building and have no other option but to rely on expert opinion.
Tags:



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East





















I would like to know where I can see these in person, see hands on not just picture? Is there a sample available or where can one be ordered than returned if it does not fit? I’m not too concerned about cost, just fit.