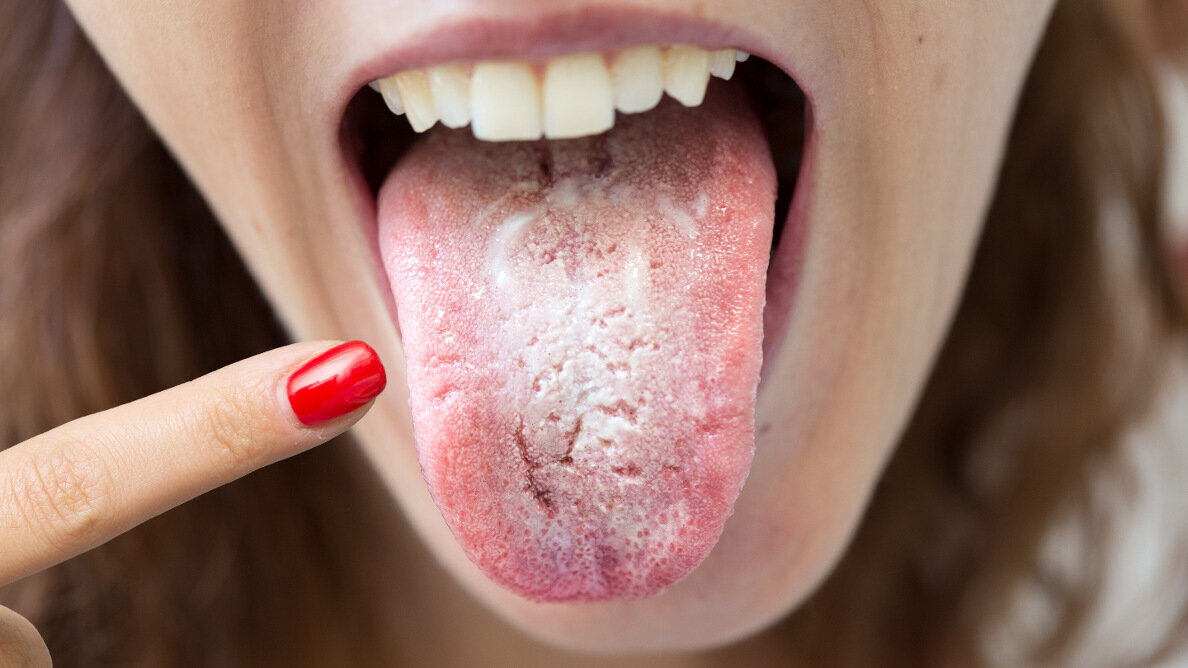
LEIPZIG, Germany: New discoveries about COVID-19 are outpacing the nomenclature. Research is emerging that suggests that a large number of COVID-19 patients experience symptoms in the oral cavity that are not yet recognised as typical signs of the disease. Geographic tongue—which is being referred to as “COVID tongue”—has been observed in those with COVID-19, as have herpetic lesions and oral aphthous ulceration.
Guidance from the World Health Organization lists the three most common symptoms of COVID-19 as being fever, a dry cough and tiredness. The oral cavity is implicated in some of the additional symptoms that the public health agency advises to watch for—such as loss of taste or smell—but it currently does not mention further oral manifestations.
Dr Tim Spector, professor of genetic epidemiology at King’s College London, has been drawing attention to symptoms of COVID-19 that present in the mouth, such as geographic tongue. He says that those suffering from “strange symptoms” like COVID tongue should stay home, even if the symptoms are not included in official lists provided by health authorities. Spector tweeted in January: “One in five people with COVID still present with less common symptoms that don’t get on the official [Public Health England] list—such as skin rashes.” He said he was seeing an increasing number of examples of COVID tongue and other strange mouth ulcers. “If you have a strange symptom or even just headache and fatigue stay at home,” he emphasised.
“One in five people with COVID still present with less common symptoms that don’t get on the official [Public Health England] list”
– Dr Tim Spector, King’s College London
In January, Spector’s Twitter feed featured numerous images of suspected COVID tongue submitted by the public. On 27 January, he shared an image of the tongue of a 32-year-old with long-term COVID-19 effects. The tongue exhibited macroglossia and scalloping at the edges, and Spector noted that specialists could not determine the cause. Dr Lucy Davenport-Jones, a consultant orthodontist from London, replied to Spector’s tweet, confirming that oral aphthous ulceration was emerging as a common complaint.
According to Spector—the principal investigator behind the COVID Symptom Study mobile application, which allows its (now more than four million) users to contribute data about the virus—at least 20 symptoms of COVID-19 are not being commonly considered. He says that 35% of people have non-classic symptoms in the first three days, when they are most infectious.
COVID-19 from the perspective of a dentist
Researchers in Iran examined the effects of the disease on the oral cavity in a review of 17 studies. They found that 170 patients, ranging in age from 9 to 90 years, had developed oral manifestations. The most common was xerostomia (reported in 75 cases), followed by dysgeusia (71 cases) and candidiasis (67 cases). Of the 67 cases in which candidiasis was identified, specimens taken from 55 of the patients confirmed fungal infection. A change in tongue sensation was reported by 48 patients, of which 28 experienced painful ulcers in the area. Muscle pain during mastication was reported by 15 patients, and ten patients experienced swelling in the oral cavity. According to the study, a change in tongue sensation correlated strongly with swollen palate and changes in the candidiasis.
The authors identified six cases of recurrent herpes simplex virus—two on the tongue and four on the hard palate. “Four patients developed erythema multiforme‐like eruptions, three of whom had palatal macules and petechiae and one of whom showed three blisters in the inner lip mucosa. Erosions, erythema, ulcers, necrotising ulcerative periodontitis, and aphthous-like lesions were also observed in single cases,” the study read.
The onset of the oral manifestations was detailed in 95 of the total 170 cases, and the researchers found a mean of 7.21 days between the onset of systemic symptoms and that of oral manifestations. The onset of the latter varied from ten to 42 days after systemic symptoms.
The authors concluded: “The oral symptoms often appeared after general symptoms such as fever and asthenia, but can still be the initial or only sign of COVID‐19. Thus, a careful clinical intra-oral examination must be performed on COVID‐19-positive patients and equally on any patients who need dental care thoroughly and systematically to ensure that no parts are missing and to obtain further clinical data, which could pave the way for further studies.”
“It is worth mentioning that these oral manifestations could be the only signs of COVID-19, and that they are also likely to manifest before general symptoms”
– Dr Pegah Hosseinzadeh, Guilan University of Medical Sciences
Corresponding author Dr Pegah Hosseinzadeh, postgraduate resident of orthodontics at the Faculty of Dentistry at Guilan University of Medical Sciences in Iran, told Dental Tribune International that it was important for dentists to check for COVID-19 symptoms in the oral cavity.
She explained: “Certainly, awareness of the symptoms, especially oral manifestations, is important to identify and manage COVID-19 patients, but also to protect the dentist and other dental patients. For this reason, dentists must stay up to date with the latest research and knowledge of mucosal COVID-19 symptoms. A careful clinical intraoral examination must be performed prior to any other dental treatment in every visit.”
Hosseinzadeh said that the study showed that COVID-19 symptoms in the oral cavity were multifactorial. She added, however, that it was certain that the immune system was playing a significant role. “Medicine, stress, opportunistic infections like candida albicans and herpes simplex, and the virus, could be considered as possible factors,” she said. “It is worth mentioning that these oral manifestations could be the only signs of COVID-19, and that they are also likely to manifest before general symptoms.”
The findings were presented in a review article, titled “COVID‐19 from the perspective of dentists: A case report and brief review of more than 170 cases”, published online on 26 December 2020 in Dermatologic Therapy, ahead of inclusion in an issue.
Spanish study finds a quarter of COVID-19 patients had oral symptoms
A cross-sectional study conducted by dermatologists in Spain in April 2020 found that a quarter of patients had one or more symptoms in the oral cavity. The study was undertaken at a temporary field hospital established to treat mild to moderate cases of COVID-19-associated pneumonia during the peak of SARS-CoV-2 infections in Madrid. It included 666 patients who had either a positive reverse transcription-polymerase chain reaction test or bilateral pneumonia.
According to the study, symptoms in the oral cavity were present in 78 cases (25.7%), and the authors listed these as follows: transient lingual papillitis (11.5%), glossitis with lateral indentations (6.6%), aphthous stomatitis (6.9%), glossitis with patchy depapillation (3.9%), and mucositis (3.9%). A burning sensation in the oral cavity was reported by 5.3% of participants and was found to be commonly associated with dysgeusia.
The study, presented in a research letter published online in the British Journal of Dermatology, stated that symptoms in the oral cavity such as glossitis or papillitis had not previously been associated with COVID‐19, but hypothesised that the contagion risk of examining the oral cavity may have prevented a thorough examination of the oral cavity of COVID-19 patients.
The authors acknowledged the study limitations that all study participants were adults with only mild to moderate COVID-19 pneumonia and that the study was conducted during a two-week period; thus, the researchers may have missed previous or later symptoms of the disease. Despite these limitations, the authors stated: “The oral cavity was frequently involved and deserves specific examination under appropriate circumstances to avoid contagion risk.”
Tags:



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East























J’ai été positif au covid 19 je ne suis plus contagieuse mais des brûlures dans la gorge et la langue et difficulté a avaler