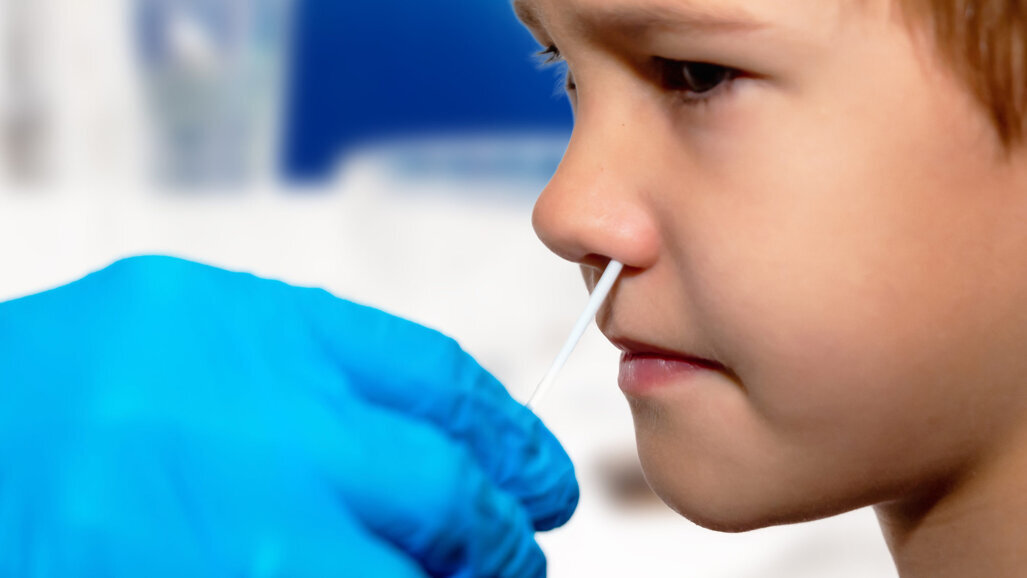
WASHINGTON, U.S.: A consortium of U.S. dental organizations has asked for federal authorization for licensed dentists to conduct SARS-CoV-2 testing in their clinics using kits approved by the U.S. Food and Drug Administration (FDA). As dentists in Utah return to work, the organizations argued that dentists have the skills to administer rapid point of care testing and that allowing them to do so will reduce infections and take pressure off the health system.
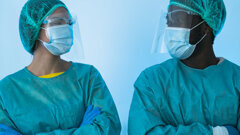
In a letter to Dr. Brett P. Giroir, assistant secretary for health at the U.S. Department of Health and Human Services, the dental organizations pointed out that, while dentists are screening their patients for COVID-19 symptoms, their clinics remain high-risk settings for the spread of SARS-CoV-2 owing to the nature of dental procedures and the risk presented by asymptomatic patients.
“Given the very high risk of COVID-19 exposure in dental settings—and the value of keeping uninfected dental patients away from hospital emergency rooms—we urge you to use your discretionary authority to extend federal authorization for licensed dentists to conduct FDA-authorized point-of-care testing for COVID-19. Doing so will reduce the need for dental patients to seek out other testing sites, except for appropriate medical referrals when indicated,” the letter read.
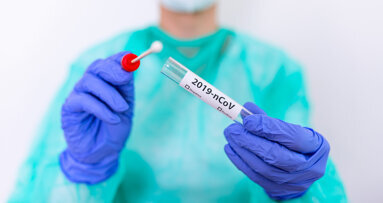
A nationwide shortage of SARS-CoV-2 testing kits has led to commercial manufacturers bringing testing kits to the market before FDA approval is granted. The organizations acknowledged the shortage, but emphasized that only FDA-approved testing kits would be reliable in preventing the spread of the virus in dental settings.
“We recognize that COVID-19 testing kits are currently scarce—and agree that they should be available when and where they are most needed (e.g., hospital emergency departments, etc.). It is worth noting, however, that there is an opportunity to alleviate the testing burden on hospital emergency departments—by testing the more than 27 million people who visit a dentist every year, but not a physician. Every one of those dental encounters is an opportunity to screen patients for COVID-19.”
Licensed dentists would need to be classified as “covered persons” under the Public Readiness and Emergency Preparedness Act so that they would be granted protection from liability associated with the administration of the tests, the organizations emphasized.
The April 22 letter was undersigned by 16 dental organizations, including the American Dental Association (ADA), Academy of General Dentistry, American Association for Dental Research and American Association of Women Dentists.
The organizations’ plea was later backed by two members of Congress, who are also practicing dentists. Republican U.S. Rep Brian Babin of Texas told District of Columbia-based media organization the Hill that he had addressed the issue with White House officials. “We would like to have the capacity to test our patients so we know who we are dealing with and the determination of what kind of procedures we should be doing and the precautions we can take,” Babin was quoted as saying. He admitted that the request ultimately “boiled down to how many of these testing kits and PPE [personal protective equipment] are available.”
Republican U.S. Rep Mike Simpson of Idaho told the Hill that making testing kits available to dentists would also help the country to reopen its economy more safely. He commented that “[Dentists] are well equipped to help our country reach the testing capacity needed to combat the spread of COVID-19. This will also help us carefully reopen the economy by keeping both patients and employees safe in the process.”
Dentists urged to be cautious as Utah reopens dental clinics
Dentists in Utah were given the green light to reopen their clinics on April 22, but patients must have their temperature taken before entering clinics. In announcing the measures, Utah Gov. Gary Herbert said that more robust measures would be in place in hospitals and surgery centers, including mandatory SARS-CoV-2 testing for all patients undergoing surgery.
“In states that are considering reopening, the ADA believes dentists should exercise professional judgment and carefully consider the availability of appropriate PPE”
– American Dental Association
At the time of writing, officials in Texas were debating whether dental clinics in the state would also reopen, and Texas Dentists for Medicaid Reform reported that regular dental services in the state may resume after April 21.
In an online bulletin, the ADA urged its members to exercise caution: “In states that are considering reopening, the ADA believes dentists should exercise professional judgment and carefully consider the availability of appropriate PPE to minimize risk of virus transmission. The ADA is communicating with the Federal Emergency Management Agency, other federal agencies, and relevant organizations to advocate that dentists, as essential health care workers, are prioritized for PPE.”
The association said that, in the absence of FDA-approved testing kits, dentists should not assume that patients who appear healthy do not have SARS-CoV-2. The ADA has issued interim guidance on the use of personal protective equipment to dentists who are considering reopening their clinics, and this is available on the association’s website.
According to data collected by the ADA Health Policy Institute (HPI) in the week of April 6, no dental clinics in Utah were open for business as usual: 5.4% of clinics in the state were open but with lower patient volumes, 89.2% of clinics were closed but treating emergency cases, and 5.4% of clinics were closed completely. In Texas, 16.8% of clinics were closed completely and 79.3% of clinics were closed but treating emergency cases. By April 26, Utah had 3,800 confirmed cases of SARS-CoV-2 and 36 associated deaths had been reported; and Texas had 25,000 confirmed cases and 651 associated deaths had been reported, according to data from Johns Hopkins University.
The HPI data showed that the U.S. states with the most widespread complete closures of dental clinics were Vermont (38.5%), Arkansas (31.1%), Pennsylvania (29.4%), New Jersey (26.6%), New York (26.6%) and California (26.7%).
LANSING, Mich., U.S.: Allowing dental professionals to test their patients for SARS-CoV-2 would decrease the high risk of transmission of the virus in ...
LEIPZIG, Germany: Researchers in India have found that scientific literature supports salivary diagnostics for SARS-CoV-2 infection as an alternative to ...
CHICAGO, U.S.: In the face of the COVID-19 pandemic, dentists have been provided with strict infection prevention and control guidelines. These include ...
LONDON, UK: Despite dental settings presenting a significantly elevated risk of infection for those in and beside the chair, testing patients for the ...
MUMBAI, India: Dentists and their patients are increasingly concerned about the elevated risk of infection with SARS-CoV-2 in dental clinics, owing to the ...
BERNE, Switzerland: The virus SARS-CoV-2 has a firm grip on the world and is affecting how people live their daily lives. In Switzerland, as in many other ...
CHICAGO, U.S.: As no studies have reported on the SARS-CoV-2-associated experiences of dental hygienists in the U.S., the American Dental Hygienists’ ...
LEIPZIG, Germany: UK health authorities have administered the first doses of the SARS-CoV-2 vaccine developed by Pfizer and BioNTech, and public health ...
CHICAGO, U.S.: In a recent study, researchers have examined the prevalence of COVID-19 in pediatric dentistry by testing children during their visit at the ...
BRUSSELS, Belgium: The provision of oral healthcare services has been severely affected all over the world by the SARS-CoV-2 pandemic because of the risk of...
Live webinar
Wed. 6 May 2026
8:00 pm EST (New York)
Ms. Ellen Karlin, Dr. Sara Karlin
Live webinar
Thu. 7 May 2026
11:00 am EST (New York)
Live webinar
Thu. 7 May 2026
12:00 pm EST (New York)
Live webinar
Thu. 7 May 2026
12:00 pm EST (New York)
Dra. Maria Carolina Erhardt, Dra. Thais Tomé Feldens
Live webinar
Thu. 7 May 2026
2:30 pm EST (New York)
Live webinar
Mon. 11 May 2026
12:00 pm EST (New York)
Live webinar
Mon. 11 May 2026
1:00 pm EST (New York)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East

































To post a reply please login or register